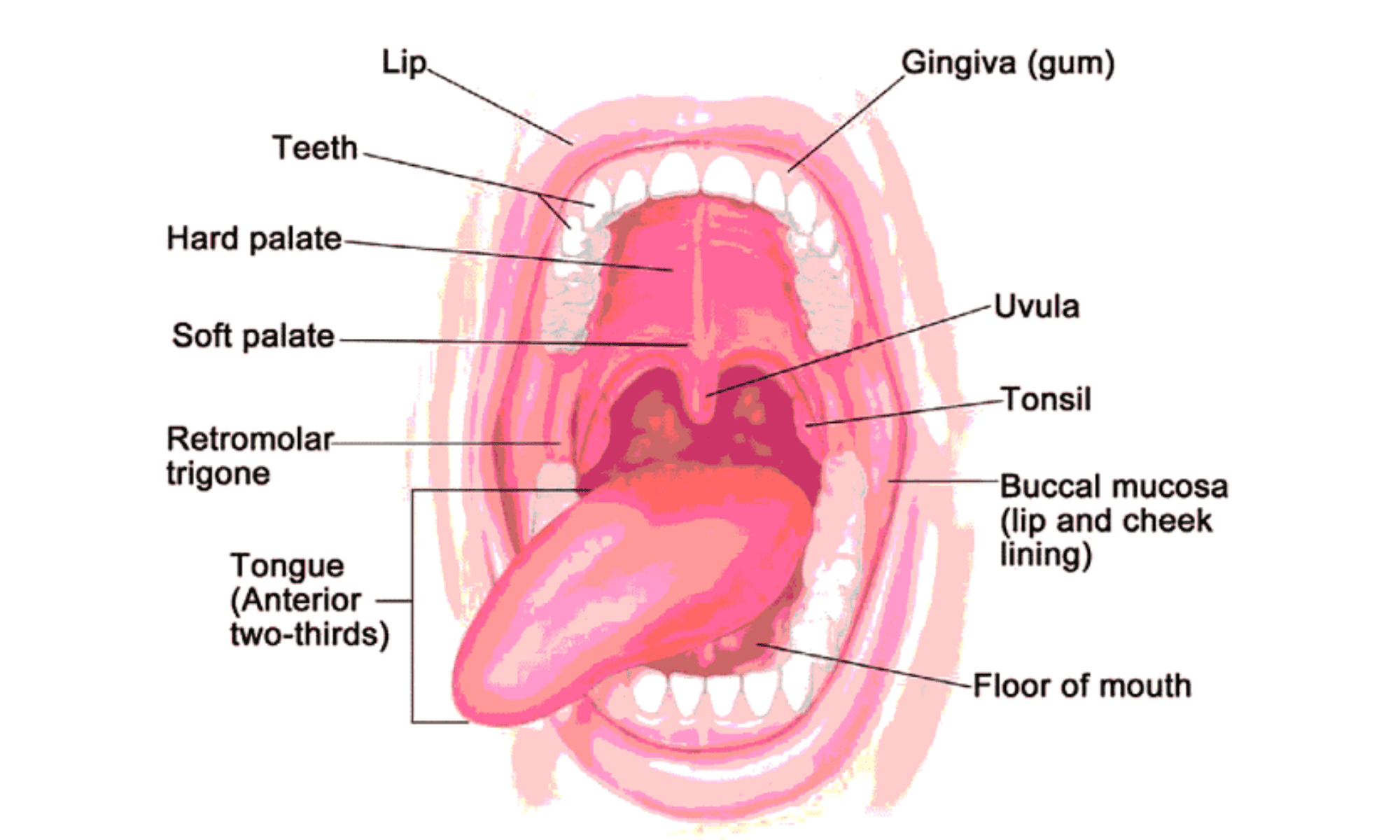
Oral cancer is a serious condition that affects the mouth, tongue, cheeks, lips, and throat. It often develops due to tobacco use, excessive alcohol consumption, HPV infection, or prolonged sun exposure (for lip cancer). Surgery is one of the primary treatments, especially when cancer is detected early. Early diagnosis and timely intervention improve survival rates and quality of life.
Condition We Treat
Our head and neck surgery team provides expert care for a wide range of conditions, including:
Cancerous and Non-Cancerous Tumors
- Oral cavity cancer (mouth cancer)
- Oropharyngeal cancer (throat cancer)
- Laryngeal cancer (voice box cancer)
- Salivary gland tumors
- Thyroid and parathyroid tumors
- Skin cancers of the head and neck

Recovery and Post-Surgery Care
The Surgical Procedure
Dr. Dushyant Mandlik specializes in advanced head and neck surgical procedures, using cutting-edge techniques to ensure the best outcomes for his patients.
Anesthesia
✔ General anesthesia is administered to ensure the patient is unconscious during the procedure.
Surgery Duration
Hospital Stay
Pre-Surgical Preparation
- Medical Evaluations: Blood tests, imaging scans, and overall health assessment to determine fitness for surgery.
- Lifestyle Changes: Patients are advised to stop smoking and drinking alcohol to improve healing and reduce complications.
- Nutrition: A balanced diet with high-protein intake supports recovery.

Types of Oral Cancer Surgery
Tumor Resection
- The primary method where surgeons remove the tumor along with a margin of healthy tissue to prevent recurrence.
Mandibulectomy (Jawbone Surgery)
- In cases where cancer affects the jawbone, part or all of the jaw may be removed and reconstructed.
Maxillectomy (Removal of Upper Jaw)
- If cancer affects the upper jaw, a portion or the entire maxilla may be removed. Prosthetics may be used for reconstruction.
Glossectomy (Tongue Removal)
- Partial glossectomy removes a portion of the tongue.
- Total glossectomy removes the entire tongue, requiring reconstructive surgery for speech rehabilitation.
Neck Dissection (Lymph Node Removal)
- If cancer has spread to lymph nodes in the neck, a neck dissection is performed to remove affected nodes and prevent further spread.
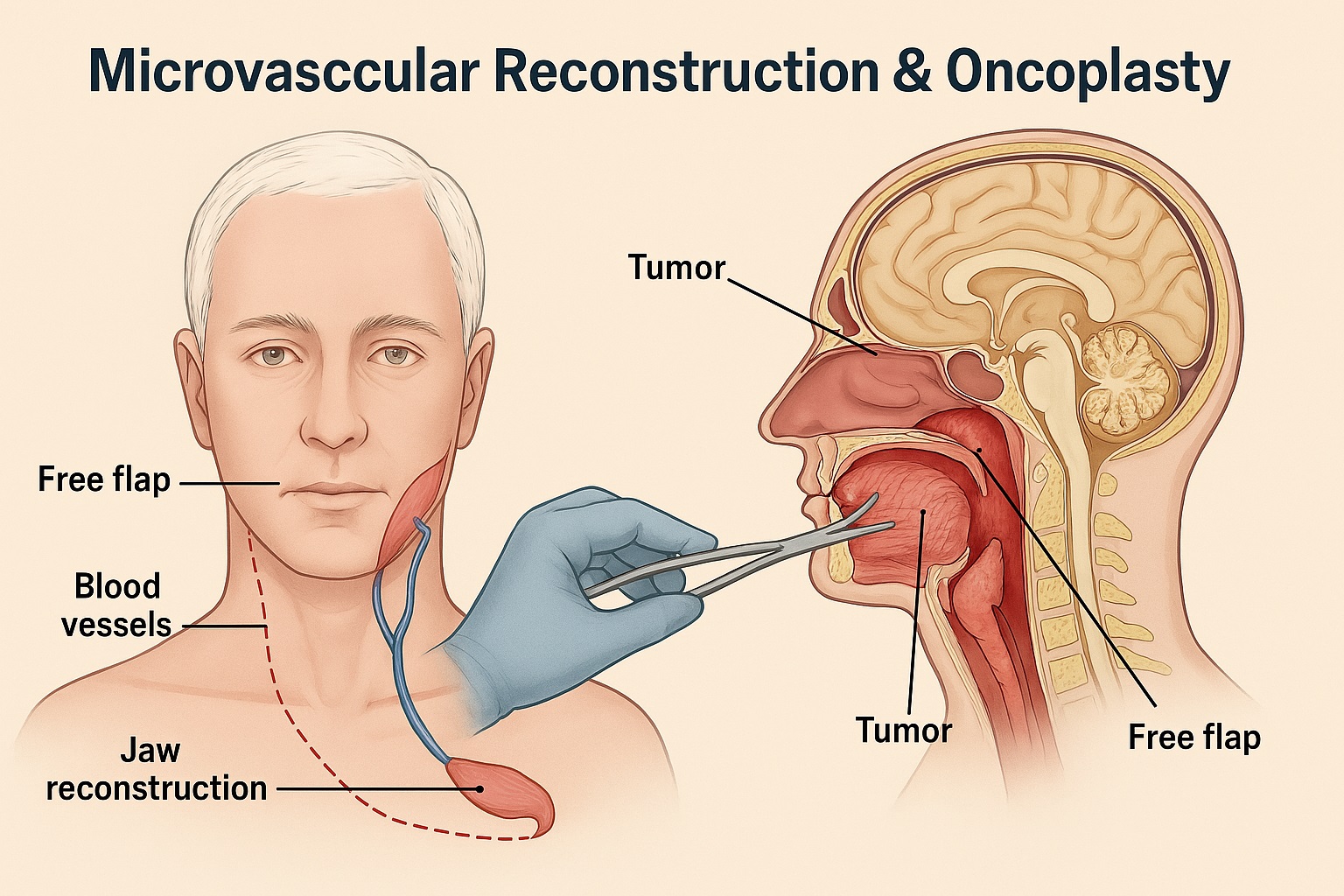
Reconstructive Surgery
- After tumor removal, reconstruction is often necessary to restore appearance and functionality. Techniques include skin grafts, bone grafts, and prosthetics.
FAQs on Oral Cancer Surgery
– Recovery varies from a few weeks to months, depending on the complexity of the surgery.
– Some patients may require feeding tubes temporarily, but most can return to a normal diet with therapy. minimally invasive procedures.
– Yes, but reconstructive procedures can minimize visible scarring.low-ups.
– Regular follow-ups, lifestyle changes, and additional treatments (if needed) help reduce recurrence risks.