Vascular tumors are a unique group of growths that arise from blood vessels. While the word tumor often causes anxiety, not all vascular tumors are cancerous, and many never require surgery. However, in certain situations, timely surgical intervention becomes crucial – not only to relieve symptoms but sometimes to prevent serious or life-threatening complications.
Understanding when a vascular tumor needs surgery, and when it can be safely observed or treated with non-surgical methods, helps patients make informed decisions and seek care at the right time.
What Is a Vascular Tumor?
A vascular tumor is an abnormal growth formed from blood vessels or lymphatic vessels. These tumors can be:
- Benign (non-cancerous)
- Locally aggressive
- Rarely malignant
They may be present at birth, appear in childhood, or develop later in life depending on the type.
Common Types of Vascular Tumors
- Hemangiomas (infantile or adult)
- Venous malformations
- Arteriovenous malformations (AVMs)
- Lymphatic malformations
- Glomus tumors
- Hemangioendotheliomas (rare, borderline tumors)
Each behaves differently, which is why treatment decisions are highly individualized.
Do All Vascular Tumors Require Surgery?
No. Most vascular tumors do not require immediate surgery.
Many are:
- Small
- Asymptomatic
- Slow-growing
- Manageable with observation or medical therapy
Surgery is considered only when the tumor causes problems, complications, or risk to vital structures.
The decision depends on:
- Symptoms
- Size and growth pattern
- Location
- Risk of bleeding
- Functional impairment
- Cosmetic concerns
- Response to non-surgical treatments
Key Situations Where Surgery Is Required
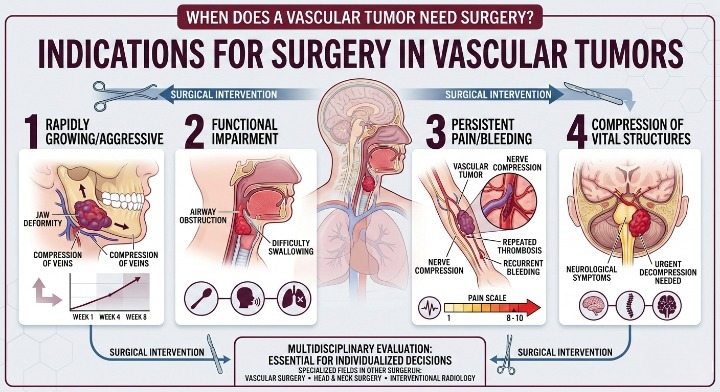
1. Rapidly Growing Vascular Tumor
A vascular tumor that shows sudden or progressive growth raises concern.
Surgery may be needed when:
- Growth is faster than expected
- Tumor begins compressing nearby structures
- There is suspicion of aggressive behavior
Rapid enlargement can lead to pain, deformity, or functional loss – especially in the head and neck region.
2. Pain That Does Not Respond to Treatment
Persistent or worsening pain is a significant indication for surgery.
Pain may occur due to:
- Stretching of surrounding tissues
- Pressure on nerves
- Repeated thrombosis (clot formation) within the tumor
If pain interferes with daily activities or sleep and does not improve with medications or minimally invasive procedures, surgical removal is often advised.
3. Recurrent or Uncontrolled Bleeding
One of the most important reasons for surgery is bleeding.
Surgery is strongly considered if:
- The tumor bleeds repeatedly
- Bleeding is spontaneous or triggered by minor trauma
- There is risk of severe blood loss
This is particularly critical for:
- Oral cavity tumors
- Nasal or throat vascular lesions
- Scalp or facial vascular tumors
In some cases, preoperative embolization is performed to reduce bleeding risk before surgery.
4. Functional Impairment
When a vascular tumor interferes with normal body functions, surgery may be necessary.
Examples include:
- Difficulty swallowing
- Speech problems
- Breathing obstruction
- Reduced vision or hearing
- Limited movement of limbs or joints
In head and neck vascular tumors, even benign lesions can significantly affect quality of life, making surgical intervention justified.
5. Compression of Vital Structures
Vascular tumors may press on critical structures such as:
- Airway
- Major blood vessels
- Nerves
- Brain or spinal cord (rare but serious)
Surgery becomes essential when compression causes:
- Breathing difficulty
- Neurological symptoms
- Reduced blood flow
- Progressive weakness or numbness
Delay in such cases can lead to permanent damage.
6. Cosmetic Deformity With Psychological Impact
While cosmetic concerns alone are not always a surgical indication, they become important when:
- The deformity is significant
- The tumor is visible on the face, neck, or scalp
- There is emotional distress or social withdrawal
In these cases, surgery may be offered after careful risk–benefit discussion, especially if the tumor is well-defined and resectable.
7. Failure of Non-Surgical Treatments
Many vascular tumors are first managed with non-surgical options such as:
- Observation
- Medications (e.g., beta-blockers for hemangiomas)
- Sclerotherapy
- Laser treatment
- Embolization
Surgery is considered when:
- The tumor does not shrink
- Symptoms persist or worsen
- Complications develop despite treatment
Surgery may also be used as a second-stage treatment after partial response to other therapies.
8. Suspicion of Malignancy or Uncertain Diagnosis
Although rare, some vascular tumors can be:
- Borderline
- Malignant
- Difficult to classify on imaging alone
Surgery is required when:
- Biopsy is inconclusive
- Imaging shows aggressive features
- There is rapid progression with systemic symptoms
In such cases, complete excision allows both treatment and definitive diagnosis.
Special Considerations in Head & Neck Vascular Tumors
The head and neck region presents unique challenges because of:
- Dense concentration of nerves and vessels
- Functional importance (speech, swallowing, breathing)
- Cosmetic visibility
Surgical decisions here require:
- Detailed imaging (MRI, CT angiography)
- Multidisciplinary planning
- Experience in vascular and head & neck surgery
Whenever possible, organ-preserving and function-sparing techniques are preferred.
Pre-Surgical Evaluation: Why It Matters
Before surgery, a thorough evaluation is essential to minimize risks.
This typically includes:
- MRI or CT scan
- Doppler ultrasound
- Angiography (in selected cases)
- Blood tests
- Assessment by anesthesia and surgical teams
Some vascular tumors require preoperative embolization to reduce blood flow and make surgery safer.
Is Surgery Always Curative?
Not always.
- Well-circumscribed tumors can often be completely cured
- Diffuse malformations may require staged or partial excision
- Some tumors may recur and need long-term follow-up
The goal of surgery may be:
- Complete removal
- Symptom control
- Functional improvement
- Prevention of complications
Success is measured not just by removal, but by preservation of function and quality of life.
Risks of Surgery for Vascular Tumors
As with any surgery, risks exist and depend on:
- Tumor size and location
- Blood supply
- Patient’s overall health
Possible risks include:
- Bleeding
- Infection
- Nerve injury
- Scarring
- Recurrence
This is why surgery is recommended only when benefits clearly outweigh risks.
When Should You Consult a Specialist?
You should seek expert evaluation if you have:
- A vascular tumor that is growing
- Persistent pain or bleeding
- Functional difficulty
- Facial or neck swelling of vascular origin
- Unclear diagnosis
- Failed prior treatment
Early consultation allows for planned, safer intervention, rather than emergency surgery.
Final Thoughts: Individualized Decision-Making Is Key
There is no single rule for when a vascular tumor needs surgery. The decision is always individualized, based on:
- Tumor behavior
- Symptoms
- Risks
- Patient expectations
- Available treatment options
With advances in imaging, minimally invasive techniques, and surgical expertise, most patients achieve excellent outcomes when treated at the right time by the right team.
If you or a loved one has been diagnosed with a vascular tumor, a head and neck cancer specialist evaluation can help determine whether observation, non-surgical treatment, or surgery is the best course of action.

